Welcome to Family Care! To help you acclimate to our practice and adjust to a new way of doing things, we thought it would be helpful to outline exactly what to expect during your first visit to Family Care. Our goal with this page is to walk you through the process of becoming a new patient, including scheduling, billing, and contact processes, as well as the expectations we’ll have for you as our patient. We hope to cover every detail that you might consider relevant during your first few appointments to our office so you’ll know what to expect and feel more comfortable during your initial visits to Family Care.
How do I make an appointment?
Call 919-544-6461 or complete this form.
When will my appointment be scheduled?
Each of our providers schedules New Patient visits at certain times during the day. You will be able to select from any available upcoming new patient appointment times for the provider you prefer. Once you become an established patient, more possible appointment times become available.
- Sabrina Mentock, MD: Not currently accepting New Patients.
- Elaina Lee, MD: Accepts 2 New Patients per week.
- Wednesdays at 9am and 11am.
- Sarada Schossow, PA-C: Accepts 14 New Patients per week.
- Monday & Tuesday at 2pm, 4pm, and 6pm.
- Thursday & Friday at 9am, 11am, 2pm, and 4pm.
- Frankee Rodriguez, NP: Accepts 14 New Patients per week.
- Monday & Tuesday at 9am, 11am, 2pm, and 4pm.
- Wednesday & Thursday at 2pm, 4pm, and 6pm.
The exact available times may vary by 30 minutes on any given day, but this is a good starting reference.
Generally, if you do not have a preference which provider or time slot you schedule, our next available new patient appointment is within 7-14 days.
Waiting List. We do have a waiting list that we keep for last minute cancellations, if you are somewhat flexible with coming in with less than 48 hours’ notice. To be placed on the waiting list, you must complete the New Patient Registration form and submit your completed New Patient Paperwork prior to your appointment. This helps us work you in for a visit quicker by having all your paperwork completed and ready to go before your visit.
To be added to the waiting list, please follow these steps:
- Complete all three New Patient Registration forms.
- Schedule an appointment for your New Patient visit.
- Ask the scheduler to add you to a cancellation list and provide alternative days or times that would be best for you. If we have any openings that match your availability, we will contact you to move your appointment to an earlier date.
What will I do before my New Patient appointment?
Before your scheduled appointment, please review these necessary steps to establish as a new patient at our office:
- Verify your insurance is active and in-network with Family Care.
- In-Network with Blue Cross Blue Shield
- Including NC State Health Plan, FEP, BlueOptions, BlueCare, BlueHome, and almost all others.
- In-Network with Cigna, United Healthcare, & Aetna
- Excluding HMOs and some third-party providers.
- Other Insurance, or Uninsured? Please reference our “Out-of-Network” policies.
- In-Network with Blue Cross Blue Shield
- Complete all three of our online New Patient forms. Start with #1 and you will be transferred to the next form after you hit Submit.
- Form 1: Demographic Information
- Form 2: Health History Information
- Form 3: Privacy Policies
- Alternatively, you can download a PDF of our full New Patient Paperwork.
- Request records from your previous provider.
- Form 4 (Optional): Records Release Form
- Alternatively, you can download a PDF to Send Records TO Family Care or Release Records FROM Family Care.
If you download a document to complete by hand, instead of completing the online version, you will need to print, complete, sign, scan, and return the documents using our File Upload page.
What will I do at my New Patient appointment?
Your very first visit to our office will be structured differently than all future visits. Because you are new to our practice, we must get you setup in our system, establish your history, and create a baseline for your future medical care. This visit will cover these specific things:
- Acute Illness & Injury. If the primary reason you are setting up a New Patient appointment is because you are sick or injured, we will address your symptoms and concerns related to an acute condition. If you are not currently sick, we’re glad you’re well! We would then skip this section and spend more time on your Future Care Plan, instead.
- Medical History. Before your visit, we rarely know anything about your medical history. This is obviously very important, so we will review all your previous diagnoses, treatments, procedures, prescriptions, and medical problems. We need this information to help you become healthier. Once you have become an established patient, we will already have this historical information documented and you will not necessarily go through this same type of review again.
- Current Medication Refills. If one of your reasons for establishing care with a new primary care provider is to continue medications that were previously prescribed by another provider, we can often prescribe these refills at your initial appointment. To take over prescribing a medication, we would first need records related to your prescription history. This includes office visit notes from your previous provider that indicate the diagnosis and condition for the medication, as well as the dates and amounts of your recent prescriptions. We cannot prescribe a medication for a chronic or long-term condition until we have this information, so you may want to ensure that your previous records are transferred prior to your appointment if this is important.
- We do not prescribe controlled substances at your New Patient appointment. There are no exceptions. After reviewing your previous records, if your provider agrees that you should start or continue a controlled medication after your visit, you may receive a prescription at your follow up visit after signing our Controlled Substance Agreement.
- Future Care Plan. After reviewing your medical history and discussing your concerns, your new primary care provider will establish a plan for your future medical needs. For most people, this involves scheduling your annual wellness exam and ordering recommended blood work to be drawn at your next appointment. If you started a new medication for a chronic illness or condition at your new patient appointment, you may be asked to follow up to check your progress after 30-180 days, depending on the medication. All new controlled prescriptions require a 30 day follow up visit.
Because of the amount of time it takes to establish you as a patient, we do not perform annual wellness exams or preventive services at your initial visit. Your New Patient visit is considered a standard, non-preventive office visit. Your preventive exam (aka. the “free” visit on most insurance plans) is usually scheduled as your second appointment to our office. This is still a “covered” service under all insurance guidelines, but it is not considered “preventive,” so any copayments and deductibles would still apply to this visit.
What changes after I have already established as a patient at Family Care?
Full Schedule Access. The reason we limit the scheduling for new patients is to ensure that our providers have the time and resources available to manage their existing patients. Each provider schedules 30-minute appointments and only has availability for a certain number of visits per week, so we want to be sure they have enough time to properly care for their existing patients. We analyze the average number of visits each patient might require per year and have calibrated each provider’s new patient volume to ensure that existing patient needs are met before we consider adding new patients.
Once you have established as a new patient, our full range of scheduling options will be open to you. Instead of selecting from 2-4 appointment times per day, you will have potential access to all 16-24 possible appointment times each day. We reserve 4 times per day, per provider, for existing patient “same day” appointments (we do not schedule these times until the same day of the appointment and only use them for acute illnesses), as well, which means you’ll usually be able to schedule a sick visit within 24-48 hours, if needed. These appointments are often taken before 10am, so call early!
Telephone / Portal Triage. We cannot provide medical advice for non-established patients, but we can help existing patients because we have an established medical history. As an established patient, you will be able to call or message our office for medical advice outside of an appointment. You will be able to call and talk about your symptoms with our nurse, and maybe seek a recommendation for an over-the-counter medication. In many cases, the advice you’ll receive may still be to schedule an appointment to fully evaluate your concerns, but you can at least talk with someone prior to the visit.
Annual Wellness Exams. You will be able to schedule your annual preventive exam. We do not perform annual wellness exams during your first visit to our office, so the New Patient visit is necessary if you’d like to schedule this appointment. This is generally advertised as the “free” preventive visit through most insurers, so we structure the appointment to comply with most insurer’s coverage standards to help you get the most out of this visit at no cost to you. For details on what this appointment covers, please read about our preventive wellness exams.
How much will my visit cost?
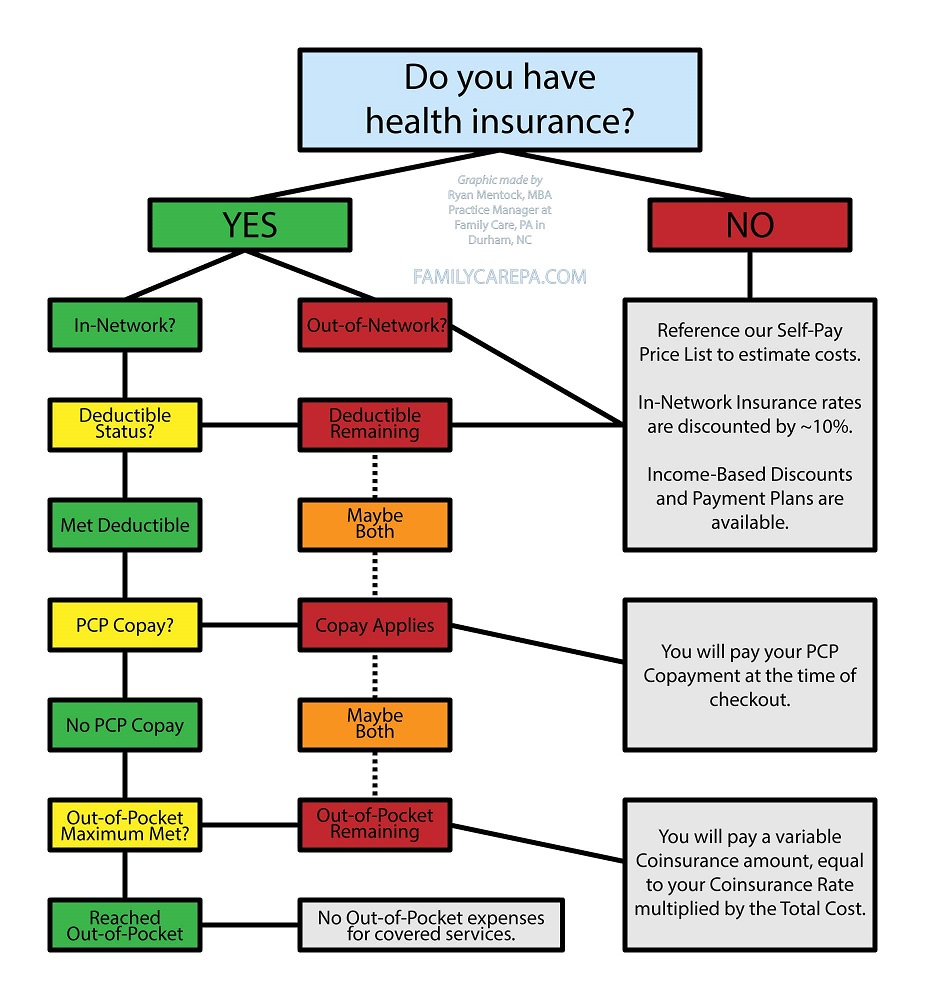
This is an important question! Unfortunately, there is no perfect answer, so we can only explain the possibilities. There are many factors that influence the cost of your visit, so hopefully this can set your expectations and help you understand how the costs are calculated. To help simplify the potential outcomes regarding your patient responsibility, we created this Flow Chart you can follow and have linked our Self-Pay Price Listing.
In general, appointments are billed based on the amount of face-to-face time you spend with your provider. New Patient appointments are generally 5%-10% more expensive than regular appointments for similar tiers of services, so your first visit is likely to be more expensive than subsequent visits. These visits are approved services by insurance (CPT 99201-99205), but they are not considered preventive. If you have a copay or deductible, that would apply to your initial visit.
A good estimate of the total cost of the visit is between $100 and $150. If you do not have insurance, or have not met your deductible, you can expect to pay this amount at checkout. If you have a co-payment, you can likely expect to just pay your co-payment amount.
If you have any additional tests (eg. EKG, flu/strep testing, etc.), you can expect additional fees for those services. These services may be covered under your co-payment, or they may be considered part of a separate “Lab-Only” deductible that many co-payment plans feature.
Basically, a short visit with no testing is relatively inexpensive, while a long visit with many tests would be relatively expensive. Most visits fall somewhere in-between, so we use ~$125 as a good starting point for your expectations, which you can adjust after considering everything you’d like to cover during your visit. If you have any specific price questions that are not available on our Uninsured Price List, please contact our office for a custom quote.
How can I verify my benefits for a New Patient Visit?
The two components of a health insurance claim are the CPT Code (what you had done) and ICD code (why you had it done). The combination of these two codes determines your level of insurance benefits. You will be billed for one of these New Patient CPT Codes:
- 99201 – New Patient Consultation, 10-15 minutes, Level 1
- 99202 – New Patient Consultation, 20-25 minutes, Level 2
- 99203 – New Patient Consultation, 25-30 minutes, Level 3
- 99204 – New Patient Consultation, 30-45 minutes, Level 4
- 99205 – New Patient Consultation, 45-60 minutes, Level 5
If you have any other services during your visit (eg. EKG, vaccines, labs, samples, etc.), you will have CPT code line items for these services, as well. In general, all the tests and services we provide are between $5 and $40, even if you didn’t have insurance at all, outside of the consults themselves.
Your ICD Code (aka Diagnosis Code) will be dependent on your reason for the visit, but it would NOT be considered a “preventive code.”
You can reference your enrollment paperwork for benefit details, obtain benefit information through your insurer’s portal, or speak with a customer service representative from your insurance over the phone. You should attempt to verify your coverage for CPT 99201-99205 when billed as a diagnostic / non-preventive service to fully understand your coverage.
What is likely to happen?
The most likely scenario for your first visit really depends on a few different factors regarding your health.
- You have no concerns or problems to discuss, you just need to establish care with a new provider.
- Your first visit will be fairly quick, with most of the time spent in discussion about your future care. We are still required to take a full medical history to establish you as a patient, even if that history is mostly blank and you have never had any serious problems. We have you complete health history paperwork and you will review the information you provided with your provider to confirm accuracy and possibly identify any gaps that were not addressed on the form. This provides a baseline for future care and will end up saving you a lot of time during future appointments. We will also identify and discuss recommended screening procedures based on your current age and responses you provide to our health history form.
- You have some minor concerns or an acute illness/injury to discuss.
- We can address and treat these immediate concerns at your first visit. Your initial consult will be focused on helping you feel better that day, but we will also review your medical history and set a baseline for future care. We will make recommendations and plans for future preventive screenings, but you may require follow-up care on your illness/injury before setting up a preventive wellness exam.
- You have some serious concerns or a major illness to discuss.
- We will begin with obtaining a detailed history of your specific issues and focus the majority of the visit on those problems. We would like to have records from a previous provider or emergency room, if possible, but that is not required. If we have those records, the visit will include a review of your previous recommendations, treatments, and diagnoses to determine if that plan has been working for you. Your future care plan will likely be focused only on these issues and preventive measures will be addressed once your immediate concerns have been stabilized or resolved.
Your initial visit is an approved service and you will be approved as a “established patient” for up to three years after your most recent visit. The visit is necessary for us gather the information we need to take care of you. For almost everyone, this is the only time you will have certain restrictions on what you are able to do during a non-preventive appointment.